The Case for Vaccines: Why They’re Important as Ever, and How to Approach Tricky Conversations About Them
Vaccines have a long history—as far back as the 11th century. They’ve become a hot-button topic over the last couple of decades, and certainly now on the cusp of the development of a COVID-19 vaccine. How do they work? Are they dangerous? Which ones should I get?
This article is here to answer all these questions and more. We’ll go over the history of vaccines, how they work, myths vs. facts, ensuring those around you are vaccinated, vaccines you need for different situations (including the risks of not getting vaccinated), and how to handle any discomfort after receiving your vaccines. You can find additional resources at the bottom of this page as well.
Fast Facts About COVID-19 Vaccines
- COVID-19 vaccinations began in the U.S. in December 2020. As of May 2021, 47.9% of the total population has received at least one dose and 37.8% are fully vaccinated. That’s 60.2% and 47.9% of adults, respectively.
- Every person 12 years of age and older in the U.S. is now eligible for COVID-19 vaccination. Pfizer is available for ages 12 and up, and Moderna and J&J/Janssen are approved for individuals who are 18 and older.
- Some companies and states are offering incentives for people to get vaccinated. Freebies include food, beer, tickets to sporting events, scholarships, and even a $1 million lottery prize for several vaccinated residents in Ohio!
- According to the New York Times Coronavirus Vaccine Tracker, 90 vaccines are being tested in human clinical trials, with 27 in the final stages of testing. Researchers are investigating an additional 77 preclinical vaccines in animals.
- The CDC reports the vaccine created by Pfizer and BioNTech SE displays 95% efficacy, and 0% of the people in the trial were hospitalized due to COVID-19 after receiving the shots. (It’s important to remember two doses are needed for the vaccine to work.)
- On the whole, COVID-19 vaccines have resulted in minimal side effects and rare allergic reactions, not unlike other vaccines. However, after a highly publicized pause of the J&J/Janssen vaccine due to a rare risk of blood clots with low platelets, the CDC has issued a warning for women under 50.
- Dr. Anthony Fauci advises that vaccinated people will likely need a booster COVID-19 vaccine eight to 12 months following their second shot.
- Per CDC guidelines, fully vaccinated individuals can resume normal activities without physically distancing or wearing a mask—unless required by local, state, federal, or business laws or regulations.
How Vaccines Work
Vaccines were developed as a way to help our natural defenses protect against and build immunity to particularly dangerous and/or deadly diseases. By releasing a small amount of the disease into our bodies via immunizations, our immune systems learn how to react to them and build up specific defenses.
Vaccines typically do not cause individuals to develop the infection they seek to fight against, but they can sometimes lead to mild general symptoms such as fever or muscle pains. These typically subside in a day or two. Once the body processes the vaccination, our T- and B-lymphocytes build up a memory of the disease and can remember how to fight against them if those cells ever enter the body again. While some vaccines last a lifetime, others, such as tetanus, require boosters from time to time.
The two main types of vaccinations given in the United States include:
Live, attenuated vaccines
This type of immunization include a weakened version of the germ that causes the specific illness/disease. Because it has been weakened and is given in such small amounts, it’s safe for the vast majority of individuals. If you’re immunocompromised or have another long-term health issue, speak with your doctor before receiving the vaccine. Typically, one or two doses of a live vaccine can provide long-term immunity.
Inactivated vaccines
This vaccine uses a killed germ from the specific disease, including Hepatitis A, Flu, Polio, and Rabies. Inactivated vaccines typically do not last as long as a live vaccine and often require booster shots across the lifespan.
Vaccines: Myths vs. Facts
Myth: Herd immunity is good enough for my child/me.
Fact: The point of vaccines is to create herd immunity—without the suffering and risk that comes from individuals contracting the disease in order to develop that immunity. Herd immunity requires between 50%-90% community immunity before becoming effective, which means that getting there through allowing the sickness to proliferate on its own needlessly puts many at risk of permanent injury or death.
Myth: Vaccines give you the disease you’re trying to prevent.
Fact: These days, the vast majority of vaccines are made with inactivated organisms making it extremely unlikely to contract the illness.
Myth: It’s better to reach immunity by getting a disease rather than being immunized.
Fact: Vaccines exist to prevent harmful and potentially deadly diseases; even illnesses such as the common flu lead to approximately 12,000 to 61,000 deaths in the U.S. annually.
Do Vaccines Cause Autism?
Put simply, no study shows autism spectrum disorders (ASD) and vaccines are linked. Per the Centers for Disease Control (CDC), several studies looked for any possible connections between vaccines themselves and vaccine ingredients—none of them found any causality.
Some people think correlation exists because the number of children diagnosed with Autism Spectrum Disorder has grown exponentially since the late 1990s. That said, autism diagnoses made between the 1940s and 1980s tended to focus only on extreme cases, while diagnoses made from the 1990s onward considered the full spectrum of the disorder.
In 1998, a group of British researchers published a Lancet report discussing potential links measles, mumps, and rubella (MMR) vaccine and ASD. The sample size they used was too small—12 children total—to be considered remotely statistically significant, and the experiments were performed without proper consent. In 2014, Lancet’s editor reported that the primary researcher, Andrew Wakefield, received funding from attorneys looking to sue vaccine manufacturers. The editor stated Wakefield’s research was “fatally flawed” and retracted the paper. Many experiments—with higher samples and appropriate consent—have been done since this initial research, and none of them have found a causal link between the MMR vaccine and ASD. The United Kingdom later banned Wakefield from practicing medicine.
Despite that initial paper being fully discredited, misinformation about the supposed connection between ASD and vaccines persists. Some people against vaccines have suggested thimerosal, a vaccine preservative, could cause autism because it contains mercury. Not only have comprehensive studies suggested the hypothesis was flawed, but most childhood vaccines don’t even contain thimerosal.
How Common Are Adverse Vaccine Reactions?
While any vaccine technically can cause an intense reaction or side effect, the chances of this happening are extremely low and rare. The CDC estimates one per every one million doses administered could potentially cause a severe allergic reaction. Most vaccines’ side effects do not extend beyond a low-grade fever or a sore muscle where you received the shot.
The federal government collects data about unwanted reactions in its Vaccine Adverse Event Reporting System (VAERS). However, the data is self-reported by anyone—not just medical professionals—and includes adverse health events that coincidentally occur after administered. This means the negative “reactions” may not be reactions at all—just bad luck and bad timing.
Like any other medication, vaccines undergo thorough and rigorous testing before hitting the market. Scientists also continually monitor the vaccines in use to ensure they remain safe and effective.
Who SHOULD Avoid Vaccines?
While vaccines are safe for the general public, the CDC advises some individuals and populations avoid them or receive them through means other than shots. Those affected by these suggestions include those who are immunocompromised, pregnant, or have had confirmed reactions in the past. However, each vaccine has its own guidelines, so ask your doctor before accepting or refusing a vaccine.
If you have a severe allergy to aluminum or neomycin, it’s best to avoid the Hepatitis A vaccination. The Tdap vaccine should receive a pass if you have epilepsy. The CDC maintains a full list of recommendations based on individual vaccines, making it easy for you to identify what will/won’t work for you.
The Vaccine Conversation: Making Sure People Around You Are Vaccinated
Vaccines save lives, so you want to ensure those around you are vaccinated so you and your family—especially those who are too young for the vaccine or have otherwise compromised immune systems—are safe. But, this conversation can be challenging to have. Here are some suggestions about how to go about them.
Speaking to Parents of Children Who Should be Vaccinated
As any parent knows, speaking with other parents or family members about their feelings on vaccinations can be difficult. At the same time, you want to ensure your children are safe and protected from common childhood illnesses if they’re around others. While the conversation may be uncomfortable, the last thing you want to happen is for your child or a compromised relative/friend to get an illness. People you should ask about their vaccination records include:
- Parents of children your kid(s) play/interact with
- Anyone planning to visit a newborn or immunocompromised person, including relatives
- Administrators regarding immunization requirements and guidelines
Some medical professionals have given suggestions about how to have this conversation—though Dr. Paul A. Offit, director of the Vaccine Education Center at the Children’s Hospital of Philadelphia, says those who reject vaccines—period, end of story—may not be reachable. So, if you encounter someone with whom you can’t discuss this, you may have some hard decisions to make.
Dr. Pooja Lakshmin advises that bringing up statistics and facts can often turn into a heated back-and-forth. So, the conversation needs to be focused on human connection instead. Dr. Sabrina H. Zubair, a pediatrician at Northwestern Medicine Central DuPage Hospital, says you should “really listen to the parents and their concerns and come at it from an objective nonjudgmental way.” Dr. Lakshmin further recommends you, “Be curious about their experience. Find out when they first started questions. What happened that made them start to think twice?”
Sometimes, the answers to these questions can provide a lot of insight. Perhaps they got conflicting information from doctors, especially if their child was born with a health condition. Maybe they fell into believing misinformation that’s been spreading about the risks. Or possibly they had a bad reaction to a vaccine themselves, and it’s got them spooked.
Chances are, this won’t be a one-time conversation. You’ll need to reiterate your own point of view and stick to your guns. While she’s speaking from a doctor’s perspective, Dr. Zubair says, “Sometimes parents need to cultivate a relationship with me and it will take a couple of months for them to trust me and follow my suggestions.” This may also apply to parents speaking to others in their lives, especially if the conversation is happening with your child’s new friends’ parents.
Sophie Jaffe, the founder of the wellness company Philosophie, says she’s “right in the middle” of the vaccine opinion spectrum, adding, “Having a right or wrong approach only creates more disconnect and lack of understanding of the other side.” In other words, trying to “win” can be detrimental to the conversation.
Medical anthropologist and researcher Eve Dubé has found some additional effective ways to have productive conversations. In addition to the advice above—listening, being empathetic, starting with open-ended questions—she says narratives work well. Those who are vaccine-hesitant often heard tragic stories that influenced their own beliefs, so a counter-story might work as a response—a story of someone whose life was saved by a vaccine. However, these are hard to come by since the normal result of vaccinations is nothing happening.
A good way to approach this, Dubé says, is to emphasize the idea of love. She’s found many people who change their minds about vaccines do so because they realize they could save the lives of those around them. For example, she’s discovered pregnant women are more likely to get vaccinated when they understand it could protect their unborn child. In another anecdote, when a woman she spoke to refused to let her newborn’s grandparents visit unless they were vaccinated against the flu, the grandparents agreed to the vaccines.
In any emotionally charged conversation, “I” statements are often useful. GoodTherapy defines this as “a style of communication that focuses on the feelings or beliefs of the speaker rather than thoughts and characteristics that the speaker attributes to the listener.” This allows you to remove blame while getting your point across, as blaming could potentially put the other person on the defensive. Be careful to not say “I” and “you” together in a negative way, e.g., “I hate that you don’t care about my child enough to get vaccinated.” Instead, aim for something like “I worry about my child’s health” or “When you say you don’t think you’re a risk to my child, I feel like I’m not being heard.”
At the end of the day, what you choose to do after these conversations is up to you. You can choose to ban any unvaccinated people from your home, refuse to allow unvaccinated people to visit until everyone in your household is fully vaccinated, or let things be. Visit refusals may cause rifts, but only you can decide what the risk/reward balance is. No matter what you choose, stand your ground unless you decide to change your mind.
Speaking to School Staff About Unvaccinated Children in Schools
In 2000, the U.S. declared measles eradicated. As the movement against the MMR vaccine gained steam, though, the disease came back with a vengeance.
From just January 1 to February 28, 2019, 206 cases of measles appeared in 11 states—70 of which were in Clark County, Washington, alone. Of those 70, 61 hadn’t been fully vaccinated, and it was discovered only 78% of their schools’ students had been vaccinated—a 95% vaccination rate is needed to ensure herd immunity. When schools had a case pop up, they had to begin an “exclusion period” of 21 days from the last time the infected child attended school, during which unvaccinated and partially vaccinated students and staff had to stay home. This resulted in 138 students in Vancouver and 293 in Evergreen being removed from schools
Obviously, this resulted in a major disruption in learning. So, schools there began to implement a program requiring proof, not just good faith, that people attending or working in schools were vaccinated.
But, on an individual level, what can you do?
To be frank—not much. Conversations with the community and staff need to be done on a policy and administrative level.
If you work in education, you know you may not be allowed to access a child’s medical history—and certainly not coworkers’ histories. This means you could have unvaccinated people around you at any time, which may be especially scary if you’re immunocompromised or otherwise unable to be vaccinated.
If you qualify for the Americans with Disabilities Act in a way that may put you at higher risk, consider asking for reasonable accommodations like having no unvaccinated kids or aides in the classroom or more frequent cleaning. While it may not be possible—the ADA mandates requests can’t cause undue hardship on the employer, and in packed and understaffed schools, shuffling kids and staff is hard—asking may open a door you thought was closed.
Healthcare Workers Talking to Patients and Colleagues
Working on the frontlines of medical care inherently means you face some health risks, but you want to know the ones that can be mitigated have been. When collecting patient health information, ask both patients and their families about their immunization records. If they have fallen behind on the immunization schedule, you can provide this information to them. You can also ask about regulations around staff vaccination requirements.
If you find out someone in your care or a peer isn’t vaccinated, consider speaking with the director of your department and/or supervisor. If you’re exposed to a preventable illness, it could also mean sharing it with other patients and/or those you love.
When you’re talking to patients about vaccines, the advice under the parents section above still stands—lead with empathy and a listening ear, providing anecdotes to illustrate points rather than overdoing it on statistics.
Begin by assuming parents will vaccinate their children. If they hesitate, provide your recommendations and answer any questions they have. If they still hesitate or refuse, you can:
- Provide them with additional information
- Stop the conversation until their next visit
- Tell them they must call ahead for any medical visits—even the emergency room—if their child is sick
- Have them sign the AAP’s Refusal to Vaccinate form, so you have a record of this refusal occurring.
Adults can be trickier, though not always. If you’re dealing with an unvaccinated adult, they may not realize they weren’t vaccinated or understand they’re still at risk at their age. They may also not be aware that they need boosters of some shots, like the DTaP, even as they age. Be sure to have a full immunization record for your patients and, if they can’t locate them, encourage them to get the vaccines just in case. Emphasize that getting these preventable diseases can negatively affect their work and social lives, risk the health of those they love (rather than just saying “other people”), and the vaccines are just as safe for adults as they are for children.
Types of Vaccines and When You Need Them
There are many, many vaccines. Some are required or recommended for all people in the U.S., while others are reserved for different circumstances. No matter the type of vaccine, as Dr. Claire McCarthy puts it, “When you don’t get vaccinated against an illness, you are more likely to catch it.”
This section delves into a comprehensive list of vaccines available in the United States, when you should get them, state mandates, and what can happen if you don’t get that vaccination. Some of the vaccinations include photos and other images illustrating what to look for when checking on symptoms.
Remember, in addition to the medical effects, you can sometimes lose your job, be denied school entry, have a doctor refuse to treat you or your child, or even be taken to court over child neglect for vaccine refusal, barring medical or other permitted concerns. State and local laws determine the specifics.
Routine Vaccines
Note: Some of the following sections contain images. All images are from Shutterstock unless otherwise noted.
- Disease It Fights: Haemophilus influenzae
- Vaccination Schedule: Three doses between 2-15 months
- When It’s Required: All 50 states and Washington DC currently require the Hib vaccination for childcare and PreK.
Diseases caused by the H. influenzae bacterium can range from mild ear infections to deadly blood infections. Some of the symptoms associated with more serious bacterial infections include belly pain, shortness of breath, trouble breathing, confusion, fever and chills, and nausea.
- Disease It Fights: Hepatitis A
- Vaccination Schedule: Two doses between 12-24 months
- When It’s Required: 22 states, one county in Arizona, and Washington DC currently have at least some requirements for the HepA vaccination for childcare and PreK
Hepatitis A is spread from person to person contact or via food or drink. Hepatitis A currently has no cure, but if you discover you’ve been exposed within the past two weeks, you can visit your doctor for a vaccination, which may help prevent the disease from becoming active. In addition to putting stress on the liver, symptoms of HepA can include pain in the right side of your abdomen, dark urine, digestion issues, feelings of weakness, nausea, jaundice, fever, and/or vomiting. Most symptoms clear up within two to six months, but liver failure and death can occur in rare instances.
- Disease It Fights: Hepatitis B
- Vaccination Schedule: Three doses between birth and 18 months
- When It’s Required: All but two states currently require the HepB vaccination for childcare and PreK. 15 states and Washington DC require this for at least some postsecondary institutions.
Hepatitis B can be contracted any time blood, semen, or other bodily fluids enter someone else’s body, including during birth or by simply sharing a toothbrush. Frighteningly, not all people with HepB show symptoms, though they can still spread it to others. This disease is divided into two categories: acute and chronic. Both inflame the liver, though acute HepB typically becomes apparent within three months of exposure with symptoms lasting up to six months, while chronic HepB can take years to show up and may signal advanced liver disease. Chronic HepB can be the result of acute HepB. Symptoms can include fever, vomiting, abdominal pain, jaundice, loss of appetite, and fatigue, among others, with HepB in particular potentially leading to cirrhosis, liver cancer, and death.
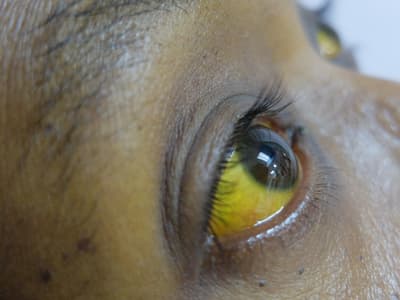
Jaundice of the eyes and skin, a common symptom of Hepatitis A and B
- Disease It Fights: Human papillomavirus
- Vaccination Schedule: Age 11-12; if you get the vaccine between 15-26, you’ll need an extra dose
- When It’s Required: Three states and Washington D.C. currently require the HPV vaccine for elementary and secondary students.
More than 100 types of HPV are currently documented, with many causing warts and a few leading to various kinds of cancer. Symptoms can include common warts on hands and fingers, genital warts, plantar warts, and flat warts. The more severe types can lead to cancers of the cervix, penis, anus, and throat—so the vaccine is now recommended regardless of gender. It can take more than 20 years for cancer to develop after exposure.
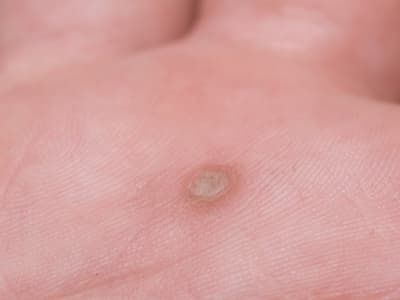
Flat wart, a common sign of HPV
- Disease It Fights: Influenza
- Vaccination Schedule: Annual vaccinations starting at six months
- When It’s Required: Seven states currently require the influenza vaccine for childcare and PreK.
This vaccine information is only about the seasonal flu. However, this vaccine also protects against H1N1 (swine flu). There is no vaccine for bird flu.
The common flu acts as a respiratory illness contagious among humans. The flu’s symptoms include fever, sore throat, cough, stuffy and/or runny nose, body and/or muscle aches, fatigue, and headaches. A small number of individuals may experience diarrhea or vomiting. While most people recover in two weeks at most, some have severe complications, such as:
- Death
- Inflamed heart (myocarditis), brain (encephalitis), or muscle tissues (myositis, rhabdomyolysis)
- Multi-organ failure
- Pneumonia
- Sepsis
- Worsening chronic medical issues, including asthma and heart disease
- Diseases It Fights: Measles, mumps, and rubella
- Vaccination Schedule: First dose 12-15 months; second dose four to six years. There is also an MMRV vaccine, which includes chickenpox—this is only available to those between 12 months and 12 years old.
- When It’s Required: All 50 states and Washington D.C. require this for those in childcare and K-12 education. If you aren’t vaccinated—or aren’t sure if you are—and are later exposed to any of these diseases, you should get the vaccine or a medication called immunoglobin within 72 hours of contact.
Note: If you were born between 1963 and 1967 or only received one round of the vaccine, you might need a new vaccination. For those born in the 60s, this is because about one million people were given what was later found to be an ineffective measles vaccine. If you’re unable to figure out if you received the ineffective vaccine or only got one round, additional MMR vaccines won’t hurt you even if you’re already immune.
Measles is more than a rash, and it can be highly dangerous to anyone who is under five, over 20, pregnant, or immunocompromised. Early signs are a high fever (up to 104° F), runny nose, and conjunctivitis. White spots on the tongue and a rash may come later. More serious complications include:
- One in five unvaccinated people are hospitalized.
- One in 20 children gets pneumonia (the most common cause of death from measles in this age group).
- One in 1,000 children develops encephalitis (which can lead to deafness or intellectual disabilities).
- One to three children die of respiratory and neurologic issues.
- Pregnant women often give birth prematurely or have a low-weight baby.
- Subacute sclerosing panencephalitis (SSPE) may develop seven to 10 years after infection—after full recovery—and this is fatal.

Measles rash
Mumps symptoms can develop between 12 and 25 days after infection, with most beginning at 16-18 days. Some are asymptomatic carriers, while others get cold-like symptoms, puffy cheeks, and a swollen jaw, the latter two being caused by swollen salivary glands. While most don’t have severe complications, some do, including:
- Inflamed testicles which may lead to decreased testicular size
- Inflamed breast tissue and ovaries
- Inflamed pancreas, brain, and tissue covering the brain and spinal cord (i.e., meningitis)
- Deafness
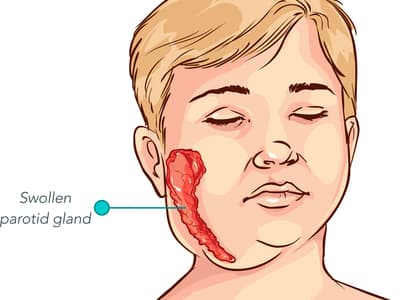
Swollen parotid gland from mumps
Rubella, also called German measles and three-day measles, typically begins with a rash on the face. Other symptoms include fever, headache, pink eye, swollen lymph nodes, cough, runny nose, and overall discomfort. Most adults have a fever, sore throat, and rash, though other symptoms may appear. About 25% to 50% of those infected won’t have symptoms, but they’re still contagious. Though the disease is usually mild, severe complications can occur, especially in women. These complications may include brain infections and bleeding issues. The problems can be worse for pregnant women’s fetuses and may involve:
- Death shortly after birth
- Hearing and vision loss
- Heart problems
- Intellectual disability
- Liver or spleen damage
- Miscarriage
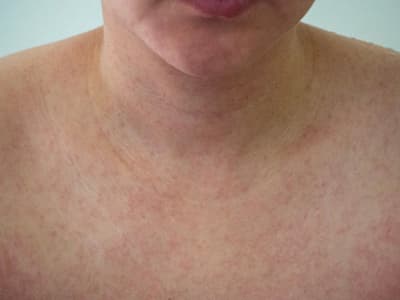
Rubella rash
- Disease It Fights: Meningococcal disease
- Vaccination Schedule: Two doses between 11-16 years old
- When It’s Required: 34 states currently require MenACWY for elementary and secondary school. 24 states require this for postsecondary institutions.
Meningococcal disease is the precursor to meningitis and can include symptoms such as fever, chills, feelings of tiredness, cold extremities, vomiting, severe pain in the chest, joints, or muscles, rapid breathing, diarrhea, and/or a dark purple rash.
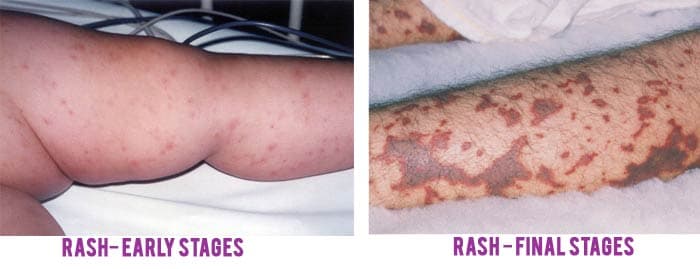
Meningococcal rash (Source)
- Disease It Fights: Meningitis B
- Vaccination Schedule: Minimum age 10
- When It’s Required: More than 30,000 high schools and 5,300 postsecondary institutions require this vaccine.
While meningococcal meningitis symptoms may begin with those that mirror the common flu, they can worsen increasingly quickly. Other symptoms you may encounter include light sensitivity, confusion, vomiting, and nausea. If left untreated, the disease can turn into septicemia or meningitis, both of which can be quickly fatal.
- Disease It Fights: Pneumococcal diseases
- Vaccination Schedule: Four doses between 2-15 months
- When It’s Required: All but nine states currently mandate the PCV vaccine for childcare and PreK.
There are two types of this vaccine: PCV 13 and PPSV 23. PCV13 is for children and adults. While kids need four shots, adults only need one. PPSV23, which is for adults, is a single-dose shot, though some people with chronic conditions may need additional rounds.
While the name may suggest otherwise, pneumococcal vaccines don’t only prevent pneumonia—it also helps stop ear, sinus, and bloodstream infections, as well as meningitis. The transmission comes from contact with saliva, mucus, and other respiratory secretions, and not everyone who spreads these diseases shows symptoms. The different types of pneumococcal diseases have different symptoms, including:
- Pneumococcal bacteremia (blood infection): Chills, fever, struggles with alertness
- Pneumococcal meningitis: Fever, headache, light sensitivity, confusion, neck stiffness, and (in babies) difficulty eating and drinking, difficulty staying alert, vomiting
- Pneumococcal pneumonia: Chills, fever, cough, rapid breathing, difficulty breathing, chest pain
- Middle ear infections: Swollen eardrum, fever, tiredness, ear pain
In severe cases, sepsis can occur as the body tries to fight off the infection. This can lead to damaged tissue, organ failure, and death.
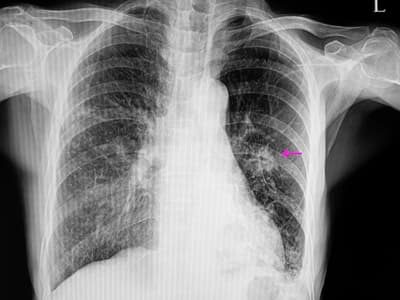
X-rayed lungs with pneumonia
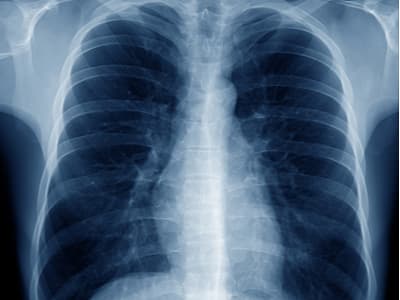
Healthy lungs for comparison
- Disease It Fights: Rotavirus
- Vaccination Schedule: Three doses between two-six months
- When It’s Required: Eight states currently require it for childcare and PreK.
Rotavirus most commonly occurs in infants and children but can also affect adults. It’s spread when fingers or food contaminated with the virus—usually by feces—are put in the mouth. Common symptoms include diarrhea, vomiting, abdominal pain, crying without tears, excess sleepiness and fussiness, and fever. Due to the dehydration caused by rotavirus, infected individuals may also deal with a dry mouth and/or throat, dizziness, decreased urination, and unusual sleep patterns. In severe cases, complications can arise, including abnormalities in multiple organ systems and death. In fact, before the vaccine, it was responsible for nearly 500,000 deaths worldwide every year.
- Disease It Fights: Shingles
- Vaccination Schedule: Two doses in adults aged 50 and older
- When It’s Required: This vaccine isn’t required anywhere, but it’s highly recommended for those over age 50.
Caused by the same virus that brings on chickenpox, shingles result in a painful and sometimes long-lasting rash. It often results in a long rash that covers and wraps around either the left or right torso and/or the face, and the rash is generally extremely painful. Individuals who get shingles once are at higher risk of reactivation due to the virus remaining inactive in the body.
There are more severe potential complications as well, including:
- Blindness if shingles are on the eye
- Death
- Encephalitis
- Hearing loss
- Pneumonia
- Postherpetic neuralgia (PHN)—affects 10% to 18% of those with shingles and involves intense pain that can last for months or years
As of July 1, 2020, Zostavax is no longer available. If you’re receiving a shingles vaccine after November 18, 2020, all remaining Zostavax has expired, and you need to insist on Shingrix.
Below, you can see the shingles rash and two rashes it’s commonly mistaken for. All should be taken seriously, but these images should help you more quickly understand what you’re dealing with.
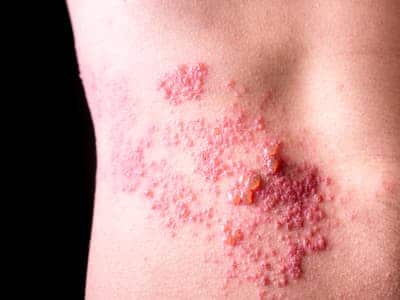
Shingles rash
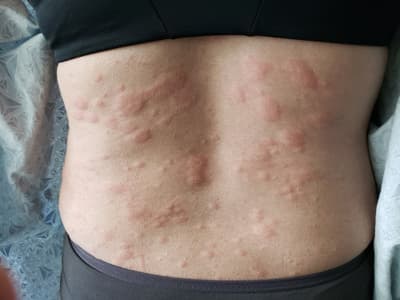
Hives rash
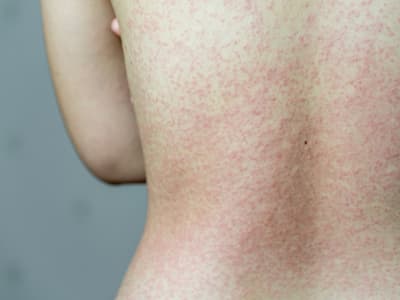
Allergic reaction rash
- Disease It Fights: Tetanus, diphtheria, pertussis (whooping cough)
- Vaccination Schedule: Five doses between two months and six years and again every 10 years thereafter
- When It’s Required: All states currently require the DTaP vaccine for elementary and secondary school. Tetanus boosters will likely be recommended after some injuries, including animal bites.
DTaP is the abbreviation for the version of this vaccine that’s given to children, while Tdap is the adult version. If some circumstances, children may receive a DT and adults may get a Td vaccine, which don’t include pertussis vaccinations. Ask your doctor about which version you need.
Tetanus is caused by injuries or infections—not just those involving rusty objects—and has an incubation period of three to 21 days (average 10). Cleaning wounds and getting infections treated promptly are key to avoiding the disease. Signs include lockjaw (jaw cramping), headache, difficulty swallowing, headache, fever, muscle spasms, and blood pressure and heart rate changes. More severe complications are:
- Laryngospasms (tightening of the vocal cords)
- Broken bones/fractures
- Additional infections
- Pulmonary embolism
- Pneumonia
- Difficulty breathing—10% to 20% of these cases are fatal
Diphtheria is spread from person to person, typically via coughing, sneezing, or touching open sores. There are two types of diphtheria: respiratory and skin. Respiratory infections look like the common cold or flu, with a sore throat, fever, weakness, and swollen glands, often followed by a toxin causing thick, gray coating in the nose and throat. This may make it hard to breathe and, if this toxin gets into the bloodstream, can result in kidney, heart, and nerve damage. Paralysis is also possible, and about 10% of respiratory diphtheria patients die. The skin infection causes open sores and ulcers but rarely results in serious complications.
More commonly known as “whooping cough,” pertussis is highly contagious and spread by coughing, sneezing, or prolonged breathing in an enclosed space. Not all people who transmit it are aware they have the disease, making it essential to be vaccinated—especially infants, who are at a high risk of complications. Symptoms usually appear within five to 10 days of exposures, though sometimes it can take up to three weeks. Early signs include a runny nose, low fever, mild cough, and apnea (in babies). After one to two weeks, fits of rapid coughing followed by a whooping sound, vomiting, and extreme exhaustion after coughing fits begin. The whooping sound is caused by a lack of air in the lungs. In between coughing fits, you may feel perfectly fine, but these fits can last ten weeks or longer—in fact, in China, this is called the “100-day cough.” Complications include:
- In babies:
- Apnea
- Convulsions
- Death
- Encephalopathy
- Pneumonia
- Half of infants under one year require hospitalization—the younger they are, the more hospitalization is likely
- In teens and adults:
- Fainting
- Loss of bladder control
- Pneumonia
- Rib fractures from coughing
- Weight loss
Additionally, those born during whooping cough outbreaks are more likely to die early, have a miscarriage, or have their infants die within the first few months.
- Disease It Fights: Chickenpox
- Vaccination Schedule: Two doses between ages one and six
- When It’s Required: All 50 states require the varicella vaccine for childcare and K-12.
It’s commonly said chickenpox is “no big deal.” And, for most people, it isn’t—but in rare cases, it can be extremely serious and even fatal, particularly for people over 15 or under one. The most notable symptom of chickenpox is the numerous red rashes that can pop up all over the body. These are typically itchy and eventually turn into scabs. Other symptoms can include headache, fever, exhaustion, and loss of appetite.
Severe complications of chickenpox include:
- Brain infection or inflammation
- Death
- Dehydration
- Hemorrhagic complications
- Pneumonia
- Sepsis
- Skin and soft tissue bacterial infections
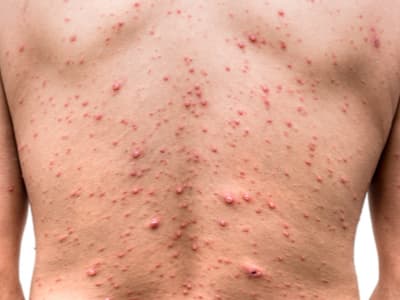
Chickenpox—see the images in the shingles section above to see how it differs from other rashes
Unique Vaccination Circumstances
The CDC especially recommends certain vaccinations if you have specific diseases or illnesses, including:
- Asplenia
- Diabetes Type 1 and Two
- Heart Disease, Stroke, or Other Cardiovascular Disease
- Hepatitis A
- Hepatitis B
- HIV Infection
- HPV
- Influenza
- Liver Disease
- Lung Disease, including Asthma
If you face any of these conditions, vaccinations become even more critically important. Vaccines strongly recommended by the CDC include:
- MMR
- Pneumococcal polysaccharide
- Renal Disease
- Shingles
- TdaP/DTaP
- Varicella
Additionally, immunocompromised people are encouraged to get the MMR, varicella, rotavirus, and shingles vaccines, as are those who live with them.
Men who have sex with men are encouraged more than other populations to ensure they receive both the Hepatitis A and B vaccinations.
Pregnant women are routinely encouraged to make sure they get both the flu shot and the Tdap vaccine.
Suppose you work as a teacher or caregiver. In that case, the Advisory Committee on Immunization Practices and the CDC recommend following the recommended vaccine schedule, including Tdap, Varicella, MMR, HPV, Pneumococcal, Hepatitis A and B, Meningitis, and the seasonal flu shot.
Travel Vaccines
To travel to certain locations, additional vaccines may be required. You need to plan far ahead for these, giving yourself at least a month—ideally more—to undergo any necessary vaccinations. If you’re a frequent traveler, it may be wise to get all necessary vaccines just in case you end up in one of the countries requiring them. You also should be fully caught up on routine vaccinations.
Below are a few of the commonly needed travel vaccinations. The CDC provides a list of destinations and any vaccines or other health concerns to be considered.
- Disease It Fights: Cholera
- Vaccination Schedule: One dose in travelers age 18-64, with potential for a booster shot
- Countries Requiring This:
- Bangladesh
- Burundi
- Cameroon
- Democratic Republic of the Congo
- Ethiopia
- Haiti
- India
- Kenya
- Malawi
- Mozambique
- Nigeria
- Philippines
- Somalia
- Sudan
- Uganda
- Yemen
- Zambia
Approximately 10% of people who contract cholera experience severe symptoms. These can include intense diarrhea, vomiting, dehydration, restlessness, leg cramps, rapid heart rate, low blood pressure, and dry mucous membranes. When dehydration becomes severe, it can result in coma, shock, and death—within hours.
- Disease It Fights: Japanese encephalitis
- Vaccination Schedule: Two doses for those aged two months and above, with seven to 28 days between each
- Countries Requiring This:
- Australia
- Bangladesh
- Brunei
- Burma
- Cambodia
- China
- Guam
- India
- Indonesia
- Japan
- Laos
- Malaysia
- Nepal
- North Korea
- Pakistan
- Papua New Guinea
- Philippines
- Russia
- Saipan
- Singapore
- South Korea
- Sri Lanka
- Taiwan
- Thailand
- Timor-Leste
- Vietnam
While only 1% of people who get Japanese encephalitis develop a clinical illness, the symptoms can be severe. These may include vomiting, headache, and fever at the start of the infection, followed by neurological changes, weakness, seizures, and other movement disorders. 20% of those who develop encephalitis die, and 30% to 50% have long-term neurologic, psychiatric, or cognitive problems.
- Disease It Fights: Malaria
- Vaccination Schedule: Four-dose schedule that can start at age five months
- Countries Requiring This:
- Afghanistan
- Angola
- Bangladesh
- Belize
- Benin
- Bhutan
- Bolivia
- Botswana
- Brazil
- Burkina Faso
- Burma
- Burundi
- Cambodia
- Cameroon
- Cape Verde
- Central African Republic
- Chad
- China
- Columbia
- Comoros
- Costa Rica
- Democratic Republic of the Congo
- Djibouti
- Dominican Republic
- Ecuador
- El Salvador
- Equatorial Guinea
- Eritrea
- Ethiopia
- French Guiana
- Gabon
- Gambia
- Ghana
- Guatemala
- Guinea
- Guinea-Bissau
- Guyana
- Haiti
- Honduras
- India
- Indonesia
- Iran
- Kenya
- Laos
- Liberia
- Madagascar
- Malawi
- Malaysia
- Mali
- Mauritania
- Mexico
- Mozambique
- Namibia
- Nepal
- Nicaragua
- Niger
- Nigeria
- Pakistan
- Panama
- Papua New Guinea
- Peru
- Philippines
- Rwanda
- Senegal
- Sierra Leone
- Solomon Islands
- Somalia
- Sudan
- Suriname
- Swaziland
- Tanzania
- Thailand
- Togo
- Uganda
- Vanuatu
- Venezuela
- Vietnam
- Yemen
- Zambia
- Zimbabwe
Uncomplicated malaria includes a cold stage and a hot stage followed by a sweating stage. Other symptoms may include headaches, nausea, vomiting, body aches, weakness, enlarged spleen, or mild jaundice, among others. Severe malaria can include seizures, coma, neurologic abnormalities, anemia, respiratory distress, blood coagulation abnormalities, kidney injury, and other symptoms.
- Disease It Fights: Polio
- Vaccination Schedule: Four doses for children, three for adults
- Countries Requiring This:
- Afghanistan
- Angola
- Benin
- Burkina Faso
- Cameroon
- Central African Republic
- Chad
- Cote d’Ivoire
- Democratic Republic of the Congo
- Ethiopia
- Ghana
- Guinea
- Malaysia
- Mali
- Niger
- Nigeria
- Pakistan
- Pakistan
- Philippines
- Somalia
- South Sudan
- Sudan
- Togo
- Yemen
- Zambia
While polio was eliminated in the U.S. in 1979—and Africa was declared free of wild polio (meaning natural passage of polio) on August 25, 2020—it’s still possible to get it throughout much of the world. The viral nonparalytic polio disease symptoms can include fever, sore throat, headache, vomiting, fatigue, pain and/or stiffness, and muscle weakness. The paralytic version may induce loss of reflexes, floppy limbs, and severe weakness or aches in muscles. Those who get polio when young may develop “post-polio syndrome,” which involves the progression of these symptoms, decreased tolerance of cold, and struggles with breathing while asleep. There is no cure for polio, and vaccination is the only way to prevent it when traveling in countries where it’s prevalent.
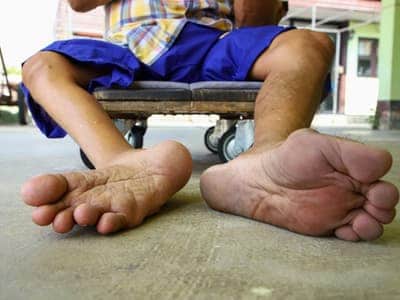
Legs of someone with polio—notice the differences in musculature and size, affecting the ability to walk
- Disease It Fights: Typhoid and paratyphoid fevers
- Vaccination Schedule: Both oral and injectable vaccines exist for people over two years old, with boosters recommended every two to five years.
- Countries Requiring This: The CDC recommends individuals get vaccinated when visiting almost all countries, especially those where outbreaks are more common—especially South Asia.
Both illnesses include a sustained fever as high as 104° F, stomach pain, diarrhea, constipation, weakness, loss of appetite, and a cough. A coated tongue is also common. Some develop a rash showing rose-colored spots. Without treatment, these diseases can be fatal. If your symptoms are gone, you may still carry Salmonella Typhi or SalmonellaParatyphi, meaning the disease could come back or be passed on—you need to have a doctor confirm you’re no longer a carrier. You shouldn’t prepare or serve food until you’ve been cleared.
Note: Typhoid and typhus aren’t the same thing—the names are similar because they were once believed to be one disease. Typhoid is spread by food that comes in contact with fecal matter; typhus is caused by flea bites. The symptoms are similar. There isn’t a vaccine for typhus.
- Disease It Fights: Yellow fever
- Vaccination Schedule: One dose typically provides lifelong immunization.
- Countries Requiring This:
- Angola
- Argentina
- Benin
- Bolivia
- Brazil
- Burkina Faso
- Burundi
- Cameroon
- Central African Republic
- Chad
- Columbia
- Cote d’Ivoire
- Democratic Republic of the Congo
- Democratic Republic of the Congo
- Ecuador
- Equatorial Guinea
- Ethiopia
- French Guiana
- Gabon
- Gambia
- Ghana
- Guinea
- Guinea-Bissau
- Guyana
- Kenya
- Liberia
- Mali
- Mauritania
- Niger
- Nigeria
- Panama
- Paraguay
- Peru
- Senegal
- Sierra Leone
- South Sudan
- Sudan
- Suriname
- Togo
- Trinidad and Tobago
- Uganda
- Venezuela
Spread by specific mosquitos types, mild yellow fever can cause vomiting, nausea, fever, and headaches. Weakness and fatigue are common and may last for several months. More extreme versions can cause problems in the heart, liver, and kidneys alongside internal bleeding. For about one out of seven people, there will be a period of remission for a few hours of a day, followed by a worse form of the illness. About 30% to 60% of those who develop a severe form of yellow fever die.
Dealing With Discomfort After Vaccines
While no vaccination should leave you in severe pain and allergic reactions are rare, it’s normal to experience some discomfort after the fact for a short while.
Injection site pain
If you face pain on your arm or other injection sites after being immunized, this is normal. If you think about it beforehand, try to relax your muscles as the shot is given; this can help reduce pain both in the moment and afterward. You may also see redness or swelling around the injection site. This is also normal. To help ease the pain, you can try putting a cool, damp towel or bag of frozen peas where you feel sore. If your doctor says it’s alright, take a non-aspirin pain reliever. While it may seem counterintuitive, it’s also a good idea to try moving your arm (or other areas where the injection was administered) around as this can help with swelling.
Flu-like symptoms
It’s also not uncommon to experience a mild fever, chills, headache, or feelings of tiredness. You should continue monitoring your temperature to ensure it doesn’t go too high, but this is rare. Drinking lots of fluids can help keep you hydrated and wearing light clothing or taking a cold/lukewarm shower can help your body stay cool.
When to get medical help
While the need for medical attention is unusual, you should stay aware of your symptoms to ensure they subside within a couple days. If redness or swelling continue to increase after 24 hours, you should call your healthcare provider. Similarly, if your temperature reaches a level your doctor states is cause for concern, check in with them. If you feel worried about yourself or your child, it’s always better to make sure everything is alright.
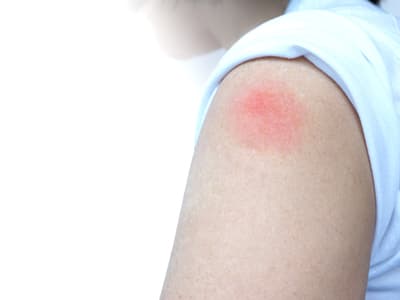
Normal injection site
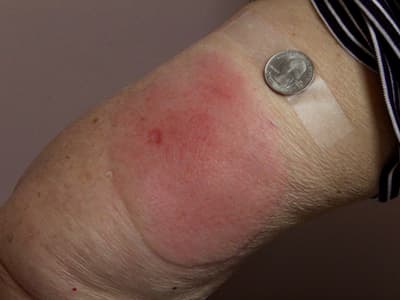
Allergic reaction at injection site
History of Vaccines
It’s common to hear, “we lived for centuries without vaccines and did just fine!” However, the need for vaccines has been known for centuries, with many attempts being made at creating them. Some of the highlights of this long history are:
- 11th Century: After surviving smallpox as a child, Emperor K’ang Hsi has smallpox scabs and scars ground up and makes his children snort them through their nostrils as a way of inoculating.
- 1716: An African enslaved man, Onesimus, tells his owner, Cotton Mather, about purposeful infection with a small amount of smallpox pus. Once he recovered from the diminished version of the illness, he was inoculated against it. Mather would later promote this method, and it became used in America and Europe.
- 1736: Benjamin Franklin’s son, Francis Folger Franklin, dies of smallpox. Franklin writes of his regret about not getting the child inoculated.
- 1738: During a smallpox outbreak in South Carolina, only 4% of those who were inoculated die, compared to 18% of the settlers and 50% of the nearby Cherokees who acquired it naturally.
- 1768: Russia’s Catherine the Great is inoculated, which encourages others to do the same after she showed no ill effects
- 1796: Physician Edward Jenner proves the hypothesis that inoculating with matter from a cowpox sore could make individuals immune to smallpox. Because cowpox was far less lethal, it led to fewer immunization-related deaths. Two years later, researchers would develop the first smallpox vaccine.
- 1820: After the smallpox vaccine, it’s observed that smallpox deaths had decreased by more than half.
- 1853: The UK mandates smallpox vaccines within the first three months of a baby’s life.
- 1897-1904: Experiments from Louis Pasteur lead to the development of live cholera vaccine and inactivated anthrax vaccine.
- 1918-1919: Spanish influenza kills more than 50 million worldwide.
- 1923: Alexander Glenny creates tetanus toxin inactivator; researchers would use the same method to generate a diphtheria vaccine three years later.
- 19401955: Jonas Salk introduces the polio vaccine; as of 2014, the disease has been eradicated in all but three countries.
- 1970s-1980s: An early anti-vaccination movement causes a pertussis outbreak in the UK.
- 1971: MMR (trivalent measles, mumps, rubella) vaccine becomes available.
- 1979: The U.S. sees its last case of polio.
- 1980: Smallpox is declared eradicated.
- 1993: Andrew Wakefield and his colleagues publish a repeatedly disproven study claiming a link between MMR vaccines and autism. Wakefield would later lose his license to practice medicine, but the myth persists, and measles rates have skyrocketed.
- Late 90s to 2000s: MMR vaccination rates drop, causing many outbreaks.
- 2019: 1,281 cases of measles were reported in 31 states, the greatest number of cases since 1992.
- 2020: COVID-19 vaccines are tested and begin to be given to healthcare workers and long-term care facilities’ residents and staff.
Sources: The History of Vaccines, History.com, Cureus, CDC—Measles Cases and Outbreaks, CDC-Polio Elimination the United States, Indian Journal of Psychiatry
Resources
Adult Immunization and the Importance of Staying Up to Date with Vaccines
If you’re on the fence about getting/maintaining your vaccinations as an adult, this informational page provides plenty of reasons why you should.
Immunization Alliance
The American Academy of Pediatrics started this group in 2008 to advocate for vaccinations, provide peer-reviewed research, and offer a place where parents can find information.
Immunization Schedules
The Centers for Disease Control provides schedules for children, adolescents, and adults so you can identify what you need to receive, how many doses are required, and when you need to schedule them.
Vaccinate Your Family
This nonprofit group works to raise the awareness of vaccine-preventable diseases and ensure individuals across the lifespan have the information and access needed to care for themselves and their families.
Vaccine Information Statements
Medical providers should give you vaccine information statements for each of the vaccines you or your child receive. The CDC also posts them online for easy access.
What to do if your child has discomfort
If your child experiences symptoms after receiving their vaccinations, use this guide from the Immunization Action Coalition for information on how to proceed.